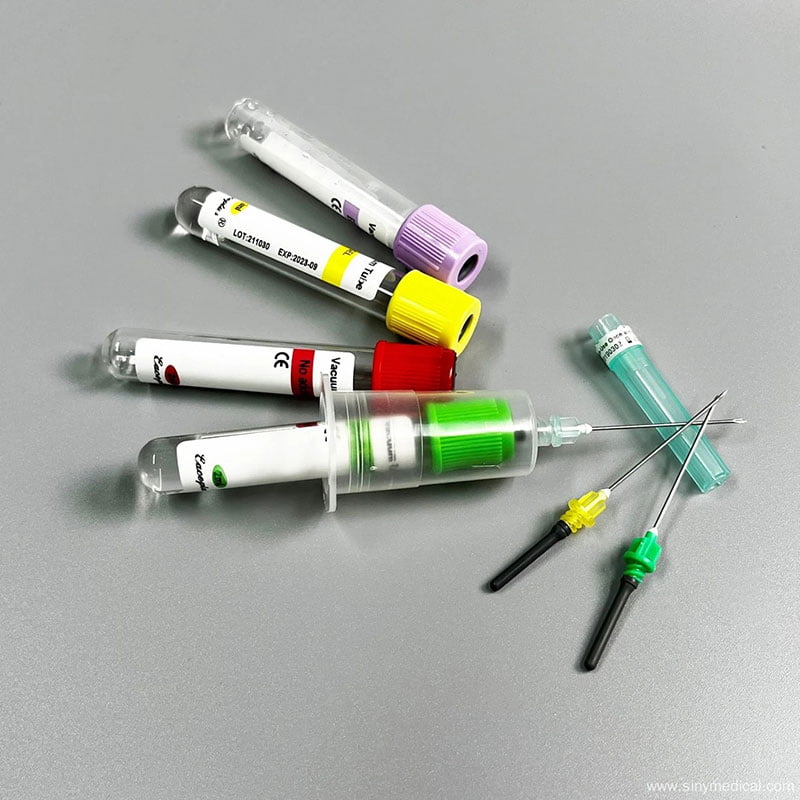
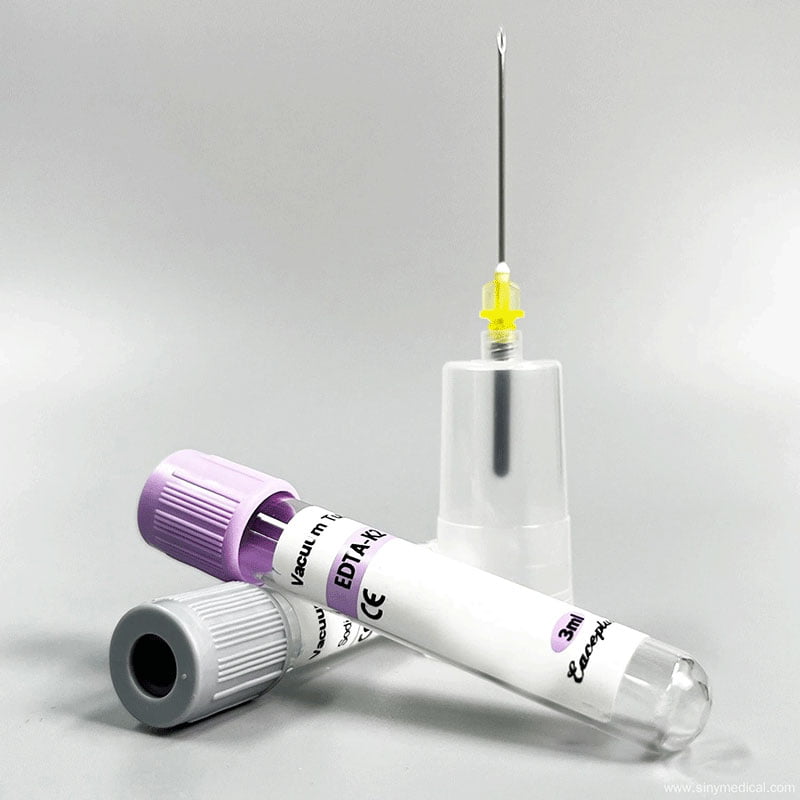
The landscape of modern healthcare relies heavily on the speed and accuracy of diagnostic results. Behind every accurate diagnosis lies a complex process of sample collection, handling, and analysis. For decades, healthcare professionals relied on traditional syringes and open needles to draw blood, a method that was often time-consuming and fraught with risks. Today, the gold standard in phlebotomy is the use of vacuum blood collection systems. These innovative devices have fundamentally transformed how medical professionals collect blood samples, ensuring that patients receive faster, more accurate diagnoses while minimizing risks.
A vacuum blood collection system is essentially a closed system consisting of a sterile needle, a holder, and an evacuated tube. The vacuum inside the tube automatically draws the precise amount of blood needed for specific tests. This automation eliminates the need for manual plunger pulling or transferring blood between containers. As a result, laboratories experience a significant boost in throughput, and the safety profile for both patients and healthcare workers improves dramatically. This article explores the profound impact of these systems on laboratory efficiency and safety, detailing why they are indispensable in contemporary medical practice.
Table of Contents
- 1 Understanding Vacuum Blood Collection Systems
- 2 Enhancing Laboratory Efficiency with Vacuum Blood Collection Systems
- 3 The Variety of Tubes in Vacuum Blood Collection Systems
- 4 The Economic Impact of Adopting Vacuum Blood Collection Systems
- 5 Quality Assurance and Global Standards
- 6 A Guide to Proper Usage
- 7 Conclusion
- 8 FAQs
Understanding Vacuum Blood Collection Systems
What Are Vacuum Blood Collection Systems?
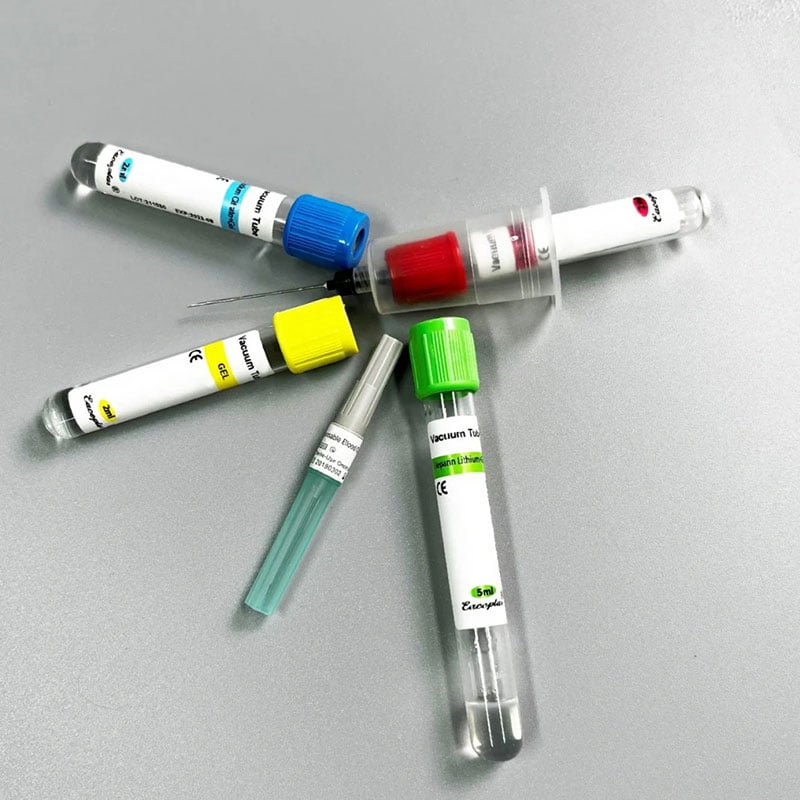
Vacuum blood collection systems are pre-sterilized, sealed tube systems designed to draw a specific volume of blood through controlled vacuum pressure. These systems consist of a double-ended needle, tube holder, and vacuum tubes containing additives or anticoagulants.
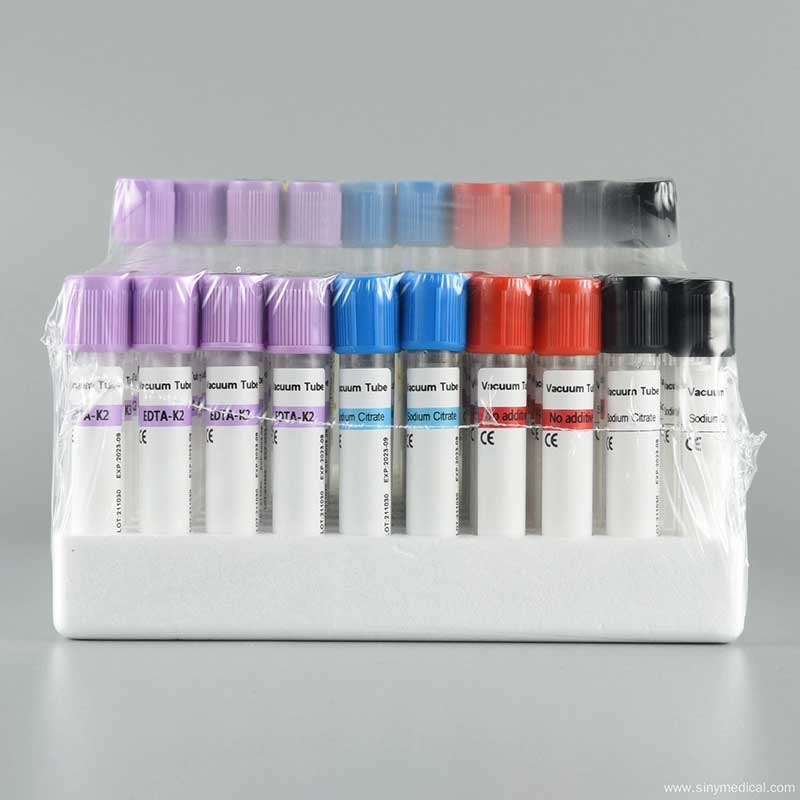
Unlike traditional syringe methods, the vacuum mechanism ensures consistent sample volume and reduces manual handling. This consistency directly improves laboratory test reliability.
Evolution of Blood Collection Techniques
Historically, blood collection tube relied on reusable glass syringes and manual transfer methods. These techniques increased contamination risk and compromised safety. With the introduction of vacuum blood collection systems, laboratories gained a safer and standardized solution.
According to blood test methodology references, standardized vacuum tubes help minimize pre-analytical errors, which account for nearly 70% of laboratory testing mistakes.
Reference: https://en.wikipedia.org/wiki/Blood_test
Enhancing Laboratory Efficiency with Vacuum Blood Collection Systems
Efficiency is the backbone of any high-functioning clinical laboratory. With the volume of patients increasing globally, labs are under constant pressure to process samples faster without compromising quality. Vacuum blood collection systems are specifically engineered to address these operational bottlenecks.
Streamlining the Collection Process
One of the most immediate benefits of using vacuum blood collection systems is the simplification of the blood draw procedure. The standardized components—a needle, a holder, and color-coded tubes—allow phlebotomists to work with speed and consistency. Unlike syringes, where the volume drawn must be estimated, vacuum tubes fill automatically to their designated volume.
Consider a situation where a patient requires multiple tests involving different additives. With a syringe, the phlebotomist must draw a large volume and carefully aliquot it into various containers. However, with a vacuum blood collection system, the phlebotomist can simply switch tubes while the needle remains in the vein.
Reducing Sample Rejection Rates
Sample rejection is a nightmare for laboratory managers. It wastes resources, delays patient care, and frustrates staff. Common reasons for rejection include insufficient sample volume, hemolysis (red blood cell breakdown), and clotted samples. Vacuum blood collection systems drastically reduce the incidence of these errors.
Because the tubes are vacuum-sealed, they fill until the vacuum is exhausted, ensuring the exact required volume is collected. This prevents “short draws” that often lead to sample rejection. Additionally, the interior of these tubes is often coated with specific additives that mix smoothly with the blood as it enters. For instance, a gentle inversion technique ensures proper mixing without causing hemolysis.
Integration with Automated Analyzers
Modern laboratories utilize highly automated machinery to analyze blood samples. These machines are calibrated to work with specific tube dimensions and additive types. Vacuum blood collection systems are manufactured to strict dimensional standards. Their uniformity allows them to be loaded directly onto automated tracks without the need for decanting or transferring specimens.
This compatibility is a key factor in lab efficiency. It eliminates the need for manual intervention between collection and analysis. If you are looking to upgrade your laboratory’s supply chain, you can explore various blood collection tubes designed for compatibility with modern analytical equipment. The standardization provided by these systems is the unsung hero of high-throughput laboratory operations.
Protection Against Needlestick Injuries
Needlestick injuries are one of the most dangerous occupational hazards for healthcare workers. A single accidental prick can transmit life-altering infections. Modern vacuum blood collection systems often integrate safety features directly into the needle design. These may include shielding mechanisms that cover the needle immediately after use or needles that retract into the holder.
Minimizing Exposure to Bloodborne Pathogens
The closed architecture of vacuum blood collection systems is the primary defense against bloodborne pathogens. In a traditional open system, transferring blood from a syringe to a tube generates aerosols—tiny droplets that can be inhaled. It also creates opportunities for spills.
This containment is essential not just during collection, but during transport and processing as well. If you want to understand the specific components that make this possible, you can learn more about the Serum Tube and its safety features.
Patient Comfort and Safety
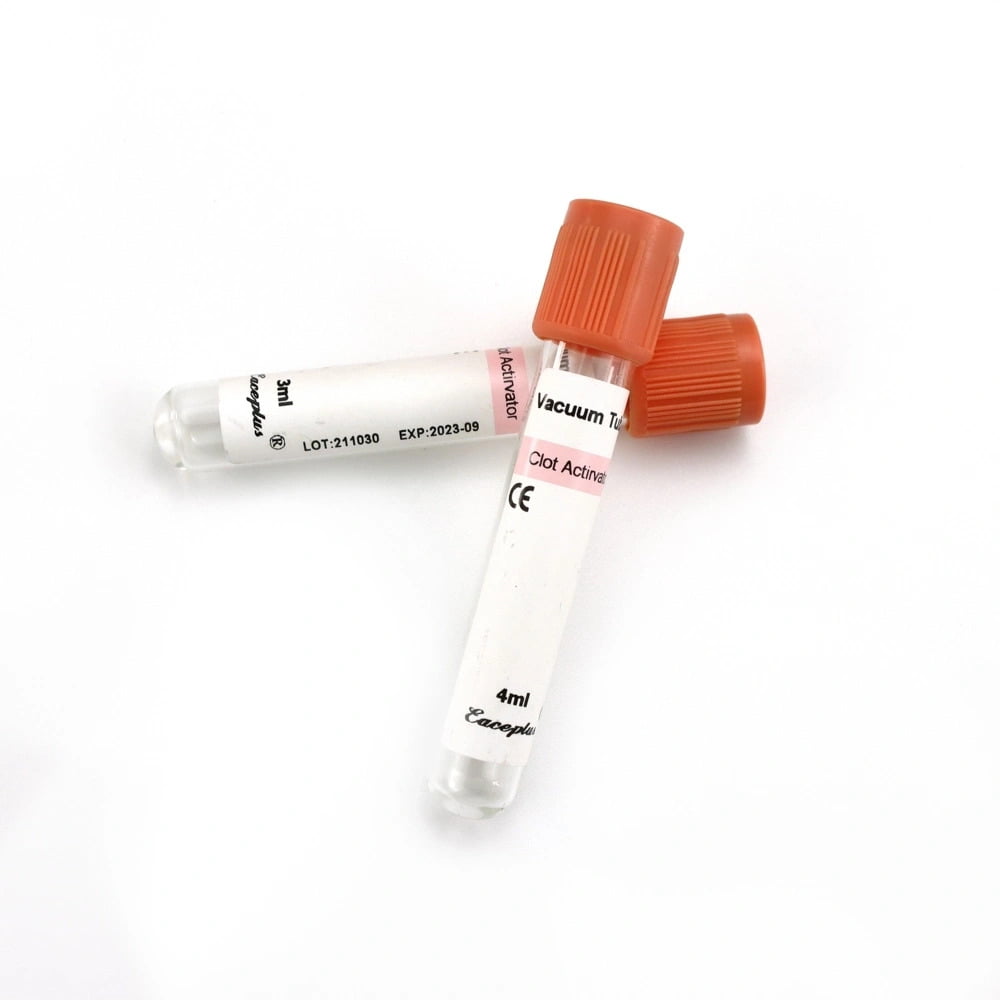
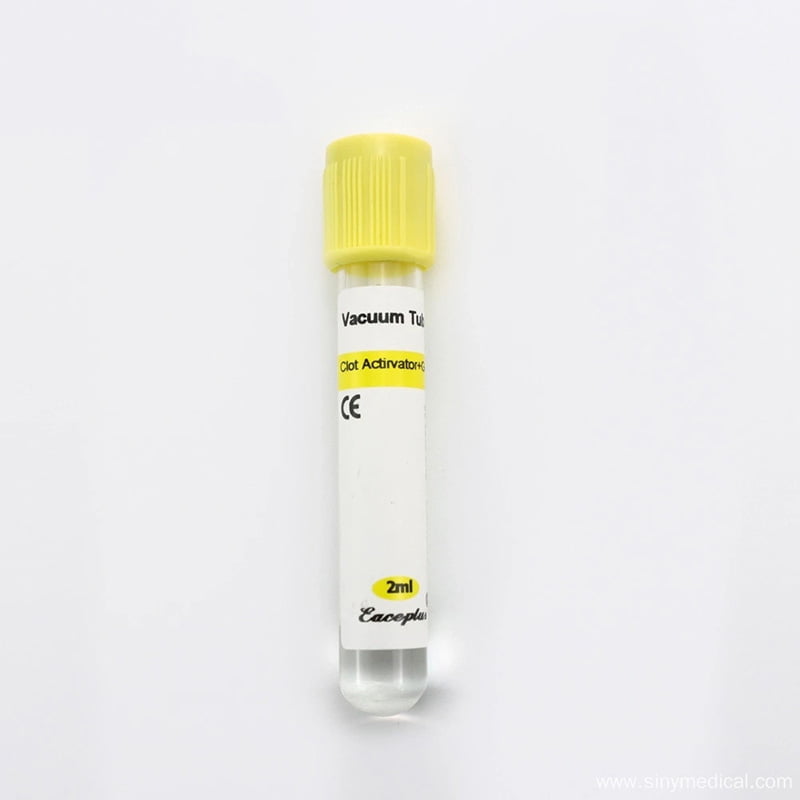
The reduced risk of hemolysis is a direct patient safety benefit. Hemolyzed samples can lead to falsely elevated readings for certain enzymes and electrolytes, potentially resulting in misdiagnosis or unnecessary re-testing. By using high-quality tubes, such as those found in the Clot Activator Coagulant Tube category, healthcare providers ensure that the sample accurately reflects the patient’s physiology.
The Variety of Tubes in Vacuum Blood Collection Systems
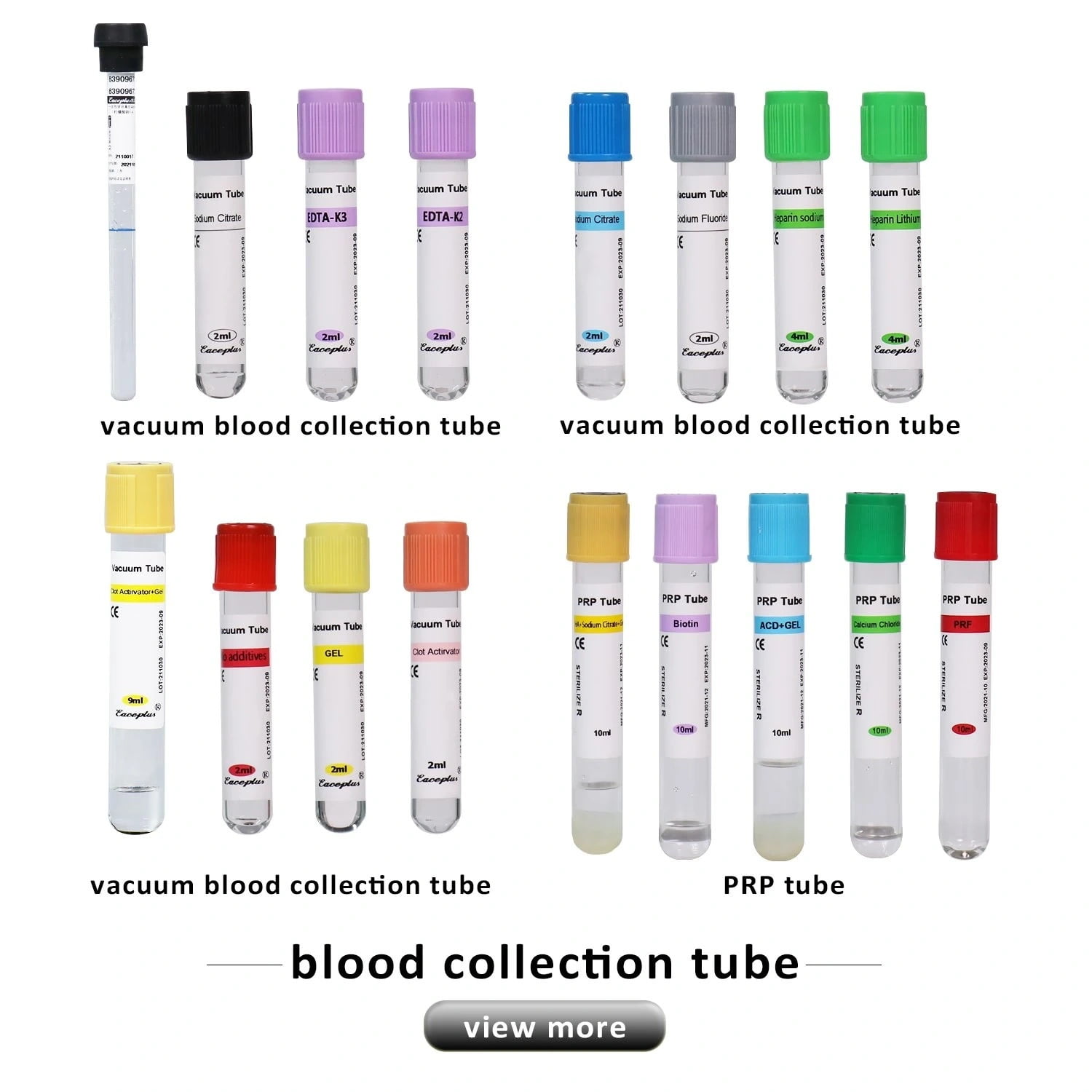
A key strength of vacuum blood collection systems is the diversity of tubes available. Each tube is designed for a specific type of analysis, identified by a color-coded stopper. This coding helps phlebotomists quickly identify the correct tube for the ordered test.
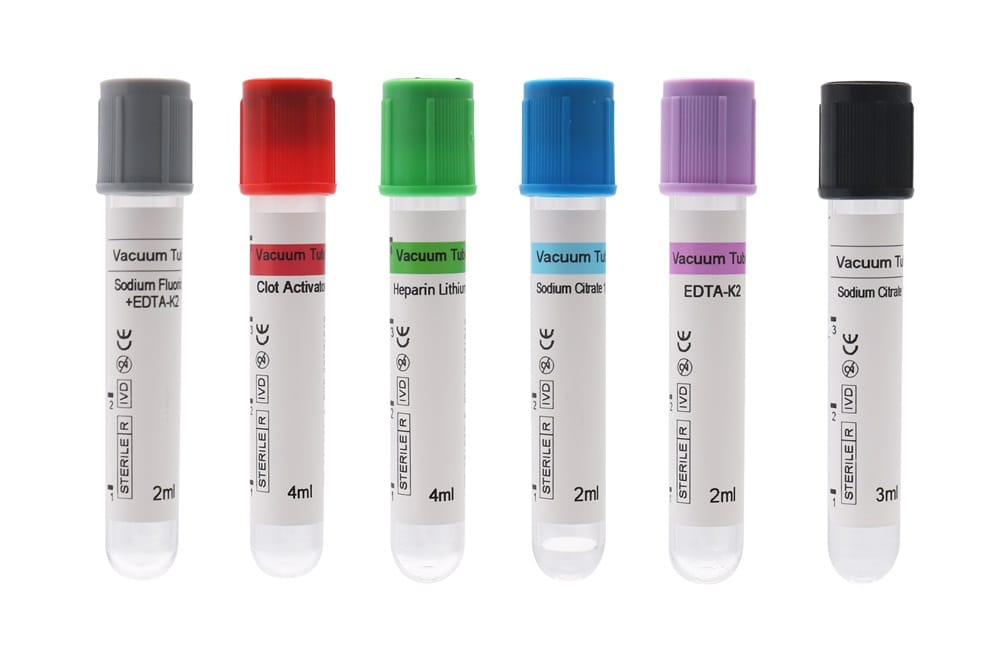
Additives and Their Functions
The interior of a vacuum tube is more than just a void; it is a pre-measured environment prepared for specific tests.
- No Additive Tubes: Often red-topped, these tubes allow blood to clot naturally. They are used for serum chemistry tests. You can find these in the No Additive Tube category.
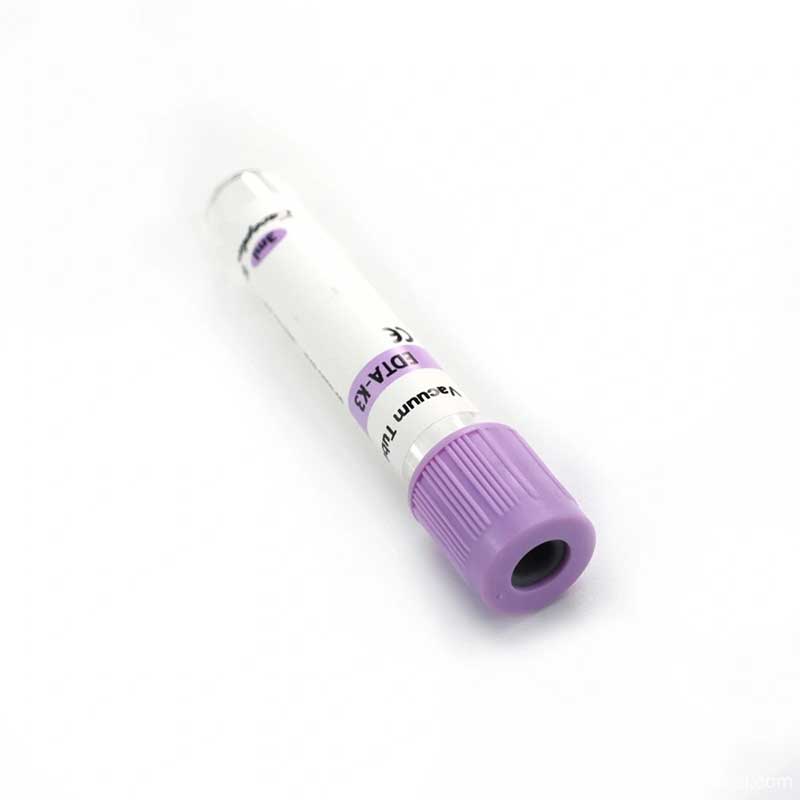
- EDTA Tubes: These are lavender or pink-topped tubes containing K2EDTA or K3EDTA. EDTA acts as an anticoagulant by binding calcium. These are essential for hematology tests like complete blood counts (CBC). For more details, you can read about The Purple EDTA Tube in the Blood Collection Tube. Siny Medical also offers a specific 2ml EDTA K2 Vacuum Blood Collection Tube.
- Sodium Citrate Tubes: Usually light blue, these tubes contain sodium citrate as an anticoagulant. They are used primarily for coagulation studies. The 3.2 Sodium Citrate Tube is a staple in any lab performing PT/INR tests.
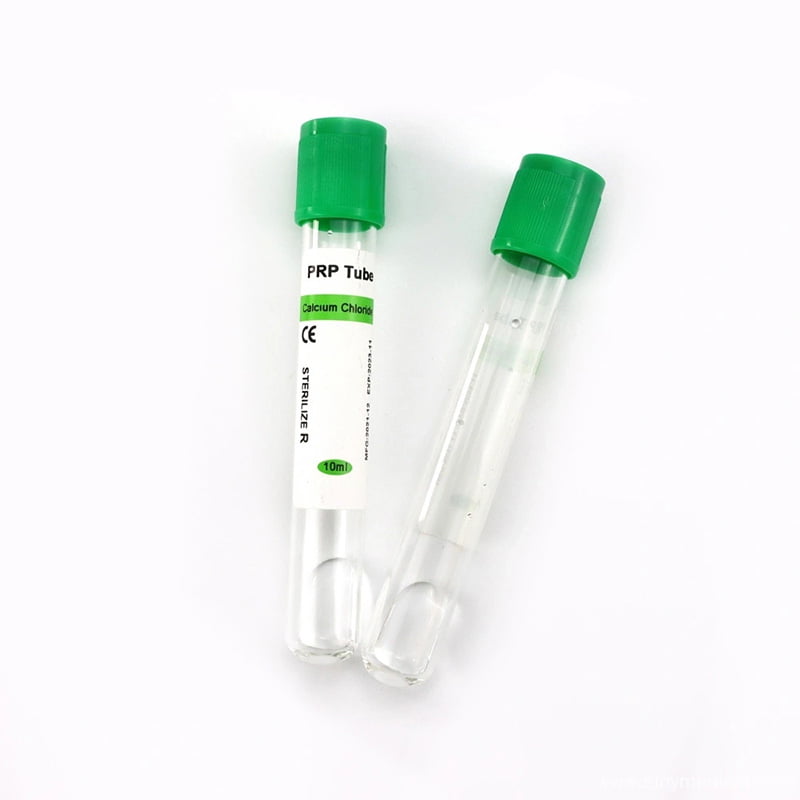
- Heparin Tubes: Green-topped tubes contain Lithium or Sodium Heparin. These inhibit thrombin formation and are used for plasma chemistry determinations. The Heparin Tube is ideal for stat tests requiring rapid plasma separation.
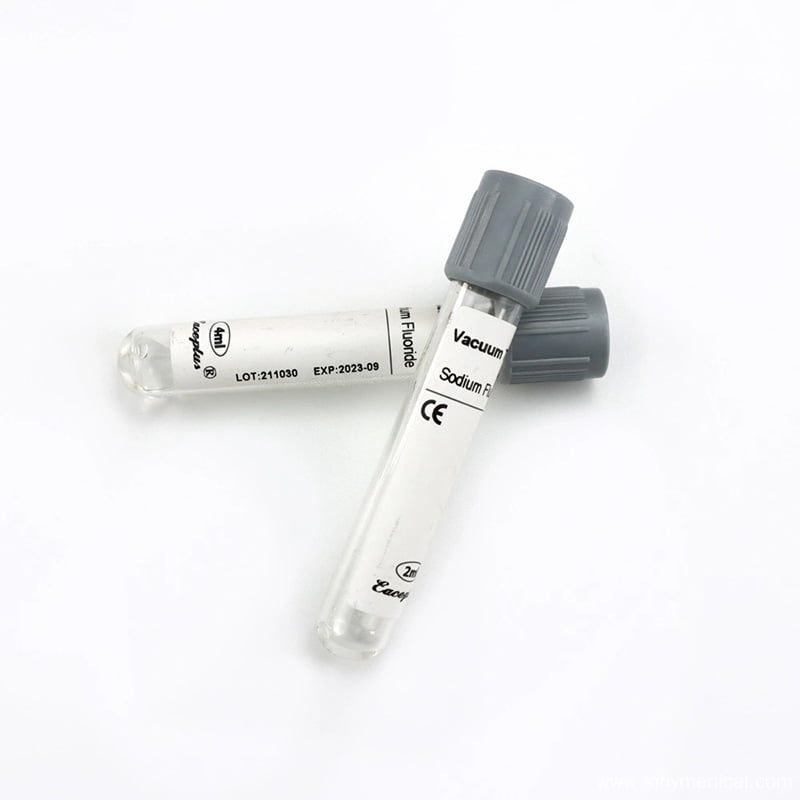
- Sodium Fluoride Tubes: Grey-topped tubes contain Sodium Fluoride, a glycolysis inhibitor, often combined with Potassium Oxalate. These are crucial for glucose testing because they preserve glucose levels for up to 24 hours. Check out the Sodium Fluoride Potassium Oxalate Tube options for glucose monitoring.
- ESR Tubes: Specific for Erythrocyte Sedimentation Rate tests, these tubes contain a specific ratio of citrate. The ESR Tube simplifies this manual test.
This variety ensures that vacuum blood collection systems can handle virtually any diagnostic requirement. Whether it is routine metabolic panels or specialized genetic testing, there is a tube engineered for the task.
Specialized Tubes for Specific Needs
Beyond the standard chemistry and hematology tubes, advancements have led to specialized products. For instance, the Micro Capillary Tube is vital for pediatric or geriatric patients where only small volumes of blood can be drawn. Furthermore, for researchers and labs dealing with trace element analysis, trace-element-free tubes are available.
It is important to choose the right manufacturer to ensure the additives are stable and the vacuum pressure is consistent. Siny Medical is one of the leading Blood Collection Tubes Manufacturers, providing a wide array of options to suit diverse clinical needs.
The Economic Impact of Adopting Vacuum Blood Collection Systems
Healthcare administrators are constantly balancing quality with cost. While vacuum blood collection systems might seem more expensive upfront compared to basic syringes, a total cost analysis reveals significant economic benefits.
Reducing Overhead Through Efficiency
Time is money in a healthcare setting. The speed at which a phlebotomist can complete a draw directly impacts staffing needs. By reducing the time per collection, vacuum blood collection systems allow existing staff to handle higher patient loads without overtime. Furthermore, the reduction in sample rejection rates means fewer re-draws. Every re-draw costs money—needles, tubes, lab tech time, and patient billing adjustments.
By ensuring a “right first time” approach, these systems lower the cost per test. Facilities can also benefit from bulk purchasing. You can explore product listings like the Disposable Sterile Blood Collection Tube to understand cost-effective procurement options.
Lowering Liability and Treatment Costs
Accidental needlestick injuries carry heavy financial burdens. They require immediate medical evaluation, potential post-exposure prophylaxis (PEP), and long-term monitoring for the exposed worker.
Additionally, accurate diagnostics prevent misdiagnosis. Treating a patient based on incorrect lab results can lead to unnecessary procedures and extended hospital stays. The reliability of a high-quality Sterile 2ml Vacuum Tube with Sodium Citrate or similar products ensures that the financial resources of the hospital are spent on actual treatment rather than correcting medical errors.
Quality Assurance and Global Standards
Not all blood collection products are created equal. For a vacuum blood collection system to be effective, it must meet rigorous international standards. Quality assurance involves checking the vacuum stability, the sterility of the tube, and the purity of the additives.
Ensuring Sterility and Stability
A compromised tube can lead to false results. For example, if a tube is not perfectly sterile, bacterial contamination can alter glucose levels or hemolyze the sample. Manufacturers must adhere to ISO standards and CE marking requirements.
When selecting a supplier, it is crucial to verify their manufacturing processes. High-quality tubes, such as the 3ml Sodium Heparin Tube or the 5ml Lithium Heparin Tube for Non-Vacuum Tube, demonstrate a manufacturer’s commitment to versatility and quality. Consistent vacuum pressure is another critical factor. If the vacuum is too weak, the tube won’t fill enough. If it is too strong, it can collapse the vein or cause hemolysis.
Supply Chain Reliability
In the wake of global health crises, the reliability of the medical supply chain has become a major focus. Hospitals need partners who can deliver consistent volumes of high-quality products. Siny Medical has established itself as a reliable partner, with a strong presence on platforms like Made-in-China. Their ability to supply diverse products, from 10ml Sodium Citrate Gel Vacuum Tubes to specialized micro-tubes, ensures that labs maintain continuity of care.
A Guide to Proper Usage
While vacuum blood collection systems are advanced tools, their effectiveness depends on proper usage. Incorrect order of draw or handling can still lead to errors.
The Order of Draw
The “Order of Draw” is a fundamental protocol in phlebotomy. It dictates the sequence in which tubes should be collected to avoid cross-contamination of additives between tubes. For instance, if a tube containing EDTA is drawn before a citrate tube for coagulation, trace amounts of EDTA could contaminate the citrate tube. This would falsely prolong coagulation times.
Understanding What are the 7 Tubes of Blood Drawn is essential knowledge for any practitioner. Generally, the order starts with blood culture bottles (if applicable), followed by light blue (citrate), red or gold (serum), green (heparin), lavender (EDTA), and grey (fluoride). Adhering to this order ensures that the vacuum blood collection system performs exactly as intended.
Mixing and Handling
Once a tube is filled, it usually requires gentle inversion to mix the additive with the blood. The number of inversions depends on the tube type. For example, a citrate tube requires 3-4 inversions, while a heparin tube might need 8-10. Vigorous shaking must be avoided as it causes hemolysis.
Training staff on these nuances is vital. For those looking to deepen their understanding of product selection, A Guide to Choosing Quality Blood Collection Tubes provides excellent insights. By following best practices, healthcare providers maximize the return on investment from their vacuum blood collection systems.
Conclusion
In summary, vacuum blood collection systems represent a cornerstone of modern diagnostic medicine. They provide a high-precision, closed-loop environment that protects healthcare workers from infection while ensuring the highest possible sample quality for the patient. By standardizing the draw volume and integrating essential additives like EDTA, Heparin, and Sodium Citrate, these systems eliminate the most common sources of laboratory error.
Whether you are a clinic manager or a laboratory technician, investing in high-quality vacuum blood collection systems from Sinymedical is a direct investment in patient safety and operational efficiency.
FAQs
1. Why are vacuum blood collection systems preferred in modern laboratories?
Vacuum blood collection systems are preferred because they improve sample accuracy, reduce contamination risk, and enhance workflow efficiency in clinical diagnostics.
2. Do vacuum blood collection systems reduce laboratory errors?
Yes, vacuum blood collection systems minimize pre-analytical errors by ensuring standardized sample volumes and closed-system handling.
3. Are vacuum blood collection systems safer for healthcare workers?
Vacuum blood collection systems improve safety by reducing exposure to biohazards and minimizing needle-stick injury risks.
4. How do vacuum blood collection systems improve diagnostic reliability?
Vacuum blood collection systems preserve sample integrity and maintain correct blood-to-additive ratios, which ensures consistent test results.
5. Can vacuum blood collection systems support automated laboratory workflows?
Yes, vacuum blood collection systems integrate seamlessly with automated analyzers and digital tracking systems, improving efficiency and traceability.